We cannot fix what we cannot confront.
So, bear with me as I delve into some hard realities within the ICU community.
I am often told, “We do early mobility in our ICU!”
However, when I probe deeper into the “mobility” provided, I find that the most common interventions that are considered mobility include:
- Chair mode in the bed
- Passive range of motion
- Hoyering to the chair/recliner
Is this mobility?
To answer that, we must first understand the key objectives of mobility that actually change outcomes. These include:
- Active engagement of the muscles
- Cognitive engagement
- Doses of gravity
Chair mode in the bed, hoyering to the chair, and passive range of motion do not actively engage patients’ brains or muscles.
These interventions change patient position, which may benefit skin integrity, lung mechanics, and the prevention of contractures, but they should not be considered early mobility.
How did this confusion arise in our culture, semantics, and practices? Here’s my theory.
In an era of absolute bed rest for everyone in the early 2000s, Polly Bailey published a study demonstrating that it was safe and feasible to walk intubated patients.
Then, in 2009, Dr. Schweikert and his team published a milestone study showing that active mobility within 72 hours of admission decreased time on the ventilator and reduced delirium by two days, while increasing the likelihood of returning to baseline function at discharge by 24%.
This finding generated excitement in the ICU community about the potential to decrease patient harm and costs.
However, standardizing the practice of having patients awake and mobile represented a radical shift and a significant challenge.
Eventually, innovative technology like ceiling lifts, in-bed arm/leg cycling devices, and safe patient handling technology emerged to support this revolution, while using early mobility as a compelling marketing strategy.
Recently, I attended a presentation on ICU early mobility. The presenter considered any movement of the patient’s body to be mobility, stating that turning, boosting, and lifting a patient were the most common forms of “ICU early mobility.”
One of the slides they used featured a table summarizing this information.
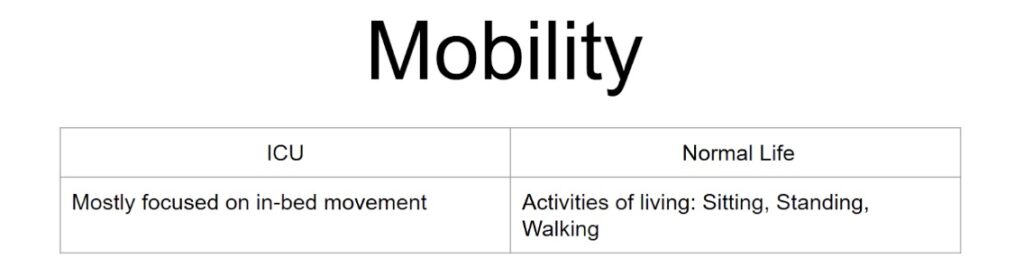
If we want to truly evaluate whether a team is practicing early mobility, it is crucial to understand what early mobility actually entails.
A patient turning themselves in bed is an example of in-bed activity with physical and cognitive engagement leading to functional activities, such as sitting at the edge of the bed, standing, taking steps, and walking.
However, much of the presentation focused on safe patient handling devices, which facilitate the passive transfer, turning, boosting, and lifting of patients – all under the label of “ICU early mobility.”
At this point, I should clarify that I deeply appreciate much of this technology and advocate for its appropriate use in the ICU.
What I struggle with, however, is the naive salesperson who quotes a 2.1-day decrease in length of stay (from the Needham 2010 study) while promoting a passive robotic leg-bike device used on sedated or weak patients who are supine in bed.
This training equipment companies provide to nurses may explain why when I ask them about appropriate mobility levels for patients, a common response is, “The chair position in the bed?”
And this may also explain why, for most patients, physicians tend to say, “Let’s mobilize them! Go ahead and sling them to the chair.”
We must be cautious about equating the benefits of having patients free of sedation, awake, and actively moving their bodies to equipment that merely facilitates positioning.
We need to stop “checking the box” for early mobility without actually providing it.
And as we approach early mobility practices, let us ask critical questions for each patient:
- What is this patient’s baseline level of mobility, and what can we do now to preserve or rehabilitate that functional capacity?
- How can we facilitate active engagement of this patient’s respiratory, core, and largest/lower muscles?
- How can we provide early and optimal doses of gravity for this patient?
- How can we cognitively engage this patient to connect with their body, family, and reality to prevent or treat delirium?
- How can we encourage this patient to mobilize and clear their secretions through their own coughing and breathing for optimal pulmonary toileting?
- What activities will help them expend energy to manage anxiety and agitation, thus protecting them from delirium and/or sedation?
If your ICU has the “early mobility” box checked, I invite you to investigate the following:
- Timing of mobility
- Level of mobility provided
- Frequency of mobility provided
- Sedation practices that hinder mobility
And while we’re at it here, let’s clarify some other misconceptions:
- Ordering physical and occupational therapy at some point during an ICU stay does not necessarily indicate the presence of an early mobility program.
- Charting “bedrest” or “chair position” may allow an ABCDEF Bundle dashboard to appear compliant, but it does not deliver life-saving care to patients.
- Having patients hoyered to the chair as standard practice may indicate that most patients have become too weak and/or confused under or from ICU care to stand and get themselves to the chair. Constantly moving patients from the lift to the chair should be a red flag, rather than a point of pride.
May we see and use early mobility as active interventions to humanize and save patients rather than a box to be checked.
May we use equipment for safe patient handling and enhancement of early mobility rather than replacement of patient engagement.
And may we standardize full compliance with the ABCDEF Bundle to have patients awake and performing their highest level of mobility as the standard, with sedation and immobility as the exception.
Want to learn how to implement true early mobility in your ICU?
Contact me for more information or join our monthly meetings for ICU Revolutionists to gain support from fellow clinicians from around the world.




