The ABCDEF Bundle is easily the best tool we have to improve patient care and outcomes in the ICU.
If you know anything about these evidence-based practices, you’re probably well aware that they can decrease length of stay and readmissions, and reduce patients’ chances of dying, while making it more likely that they’ll return to their normal quality of life after leaving the hospital.
These few benefits only scratch the surface of the importance of these practices, but even still, the majority of ICUs have not implemented them.
So, why is it that so many hospitals have failed to apply these life-saving protocols?
As I’ve learned during my time as a clinician and a consultant, there are many reasons for this, but I think one of the main ones is a lack of understanding, particularly when it comes to the financial benefits of the ABCDEF Bundle.
I’m happy to say that today, many ICU clinicians have at least some awareness of the benefits that these practices provide for their patients, but most financial stakeholders are unaware of the financial benefits of applying the ABCDEF Bundle in the ICU.
This represents a big part of the reason why we’re still seeing so much resistance to the use of these practices, as the perception is that even though they can drastically improve patient care and outcomes, their implementation will be incredibly costly.
But adopting the ABCDEF Bundle shouldn’t be seen as an expense, and the truth is, applying these evidence-based practices can help you to save much more money than it would cost to actually implement them.
So, if you’re looking to invest in the wellbeing of your patients while boosting your ICU’s bottom line at the same time, then I hope you keep reading.
Because in this article, I’m going to explain what the ABCDEF Bundle is, explore the financial consequences of not implementing these practices, and discuss the financial benefits that they can provide for your ICU.
What Is the ABCDEF Bundle?
By this point, I hope you’re already familiar with the ABCDEF Bundle.
But for those of you who aren’t quite sure what it is, or need a bit of a refresher on these evidence-based practices, I felt it was important to explain.
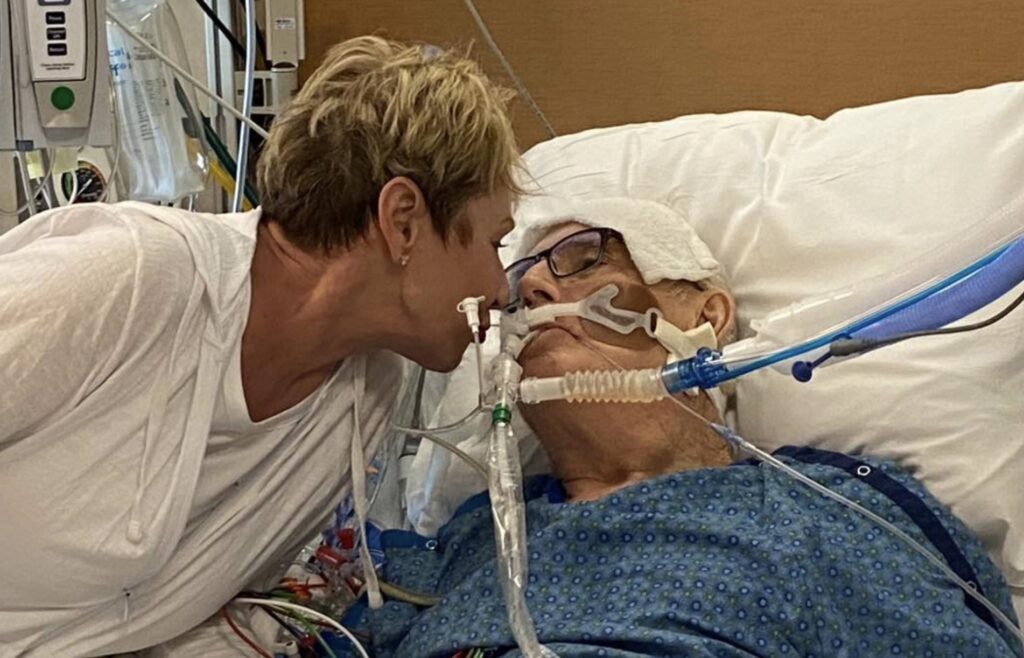
The ABCDEF Bundle, also known as the ICU Liberation Bundle, is a set of evidence-based practices used in critical care medicine to improve the care and outcomes of critically ill patients, particularly those who are mechanically ventilated.
Each letter in the bundle represents a specific element of care aimed at reducing the harmful effects of prolonged sedation, immobility, and extensive intensive care unit stays, such as delirium, ICU-acquired weakness, and ICU-acquired PTSD. The ABCDEF Bundle includes the following components:
A) Assess, Prevent, and Manage Pain
This involves assessing pain using patient reported pain scales when patients are able to report pain, or utilizing observational pain tools to assess and monitor pain levels.
Pain is then adequately treated using the PADIS guidelines to use opioid and non-opioid medications as well as non-pharmacological interventions to manage pain.
B) Both Spontaneous Awakening and Breathing Trials
Daily awakening and breathing trials involve the routine cessation of sedation and ventilator support to assess for continued need for sedation and/or mechanical ventilation.
Awakening trials should be done as soon as there is no longer an indication for sedation and at least daily when an indicator for sedation has been present.
C) Choice of Analgesia and Sedation
The ABCDEF Bundle encourages the use of pain management techniques and sedation strategies that minimize the use of opioids and sedative medications, which can contribute to delirium and prolonged mechanical ventilation.
This step should guide clinicians to ask after each intubation, each day, and for each patient, “Is there an indication for sedation? And do the potential benefits outweigh the significant risks of sedation?”
D) Delirium: Assess, Prevent, and Manage
This component focuses on assessing and addressing delirium in ICU patients.
Delirium is a state of acute confusion and altered mental status that can be common in critically ill individuals, particularly those who’ve been sedated for long periods of time.
Strategies for preventing and managing delirium include using validated assessment tools, avoiding deliriogenic medications such as sedatives, addressing underlying causes, and promoting a calm and structured environment.
E) Early Mobility and Exercise
This part of the bundle promotes early mobilization and physical therapy for critically ill patients.
Encouraging patients to move, even while they’re still on mechanical ventilation or have limited mobility, can help prevent muscle weakness and improve overall functional outcomes.
F) Family Engagement and Empowerment
Recognizing the importance of involving the patient’s family in their care and decision-making process, this component encourages communication with family members, providing them with information and support, and involving them in the care plan whenever it’s appropriate.
Families are also powerful tools to prevent and treat delirium and are therefore encouraged to be engaged with the patient as much as possible, without visiting hour restrictions.
Implementing these practices is associated with better patient outcomes, shorter ICU stays, reduced delirium and weakness, and improved long-term quality of life for survivors of critical illness, among many other benefits.
As a result, an increasing number of clinicians in critical care settings are beginning to adopt the practices described in the ABCDEF Bundle as a framework to guide their care practices and improve the overall patient experience.
That being said, the benefits of these evidence-based practices extend far beyond patient care and outcomes, and can actually confer significant financial benefits to the institutions that implement them.
What Are the Financial Consequences of Not Applying the ABCDEF Bundle?
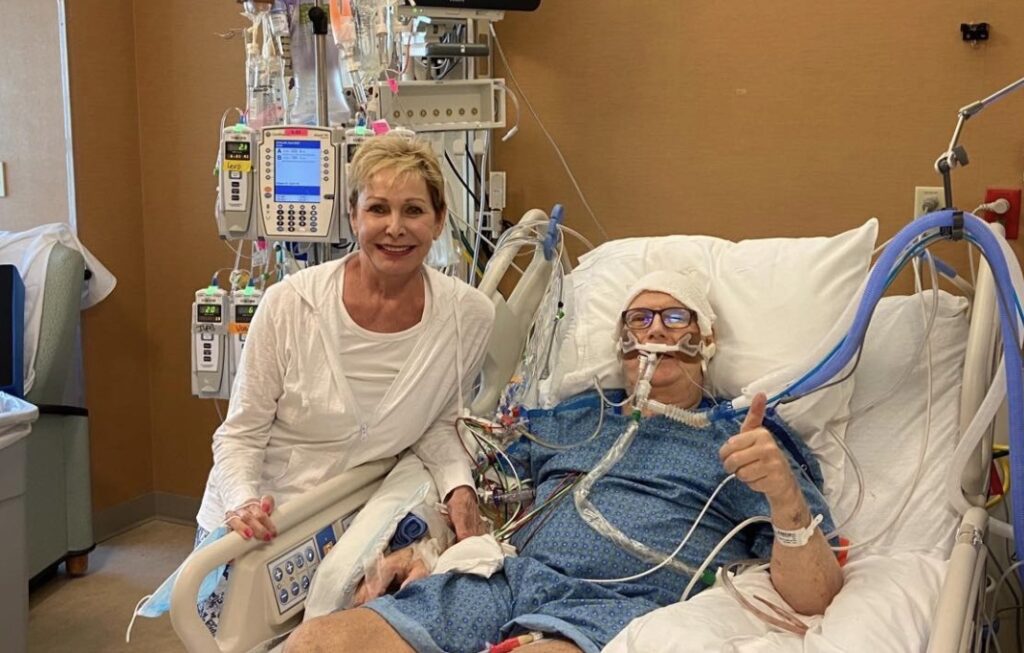
Unfortunately, there are still far too many clinicians out there who believe the myriad myths and misconceptions about the ABCDEF Bundle, like the idea that it’s an unaffordable expense.
But in reality, ICUs that choose not to implement these evidence-based practices can end up suffering some serious financial consequences.
So, before we look at the financial benefits of the ABCDEF Bundle, let’s take a look at some of the problems that can be caused by choosing not to adopt these practices. This includes things like:
- Increased time on the ventilator
- Increased delirium
- More ICU and hospital readmissions
- Patients needing to be discharged to care facilities for weeks to months of rehabilitation
- More hospital-acquired infections, such as hospital and ventilator-associated pneumonia, central line-associated bloodstream infections, and catheter-associated urinary tract infections
- More hospital-acquired pressure injuries and falls
- Increased injuries to staff
- Increased workload for staff
- Heavier psychological burden on staff, leading to burnout
What’s more, evidence continues to mount, which shows that:
- Sedation increases the risk of delirium by over eight times.
- Immobility and bed rest can significantly increase the risk of delirium.
- Delirium increases healthcare costs by 39%.
- Delirium increases time in the hospital by 4.77 more ICU days and 6.67 more hospital days, on average.
- Delirium can double the nursing hours required for care.
- Delirium significantly contributes to the psychological burden on nurses.
- Failure to mobilize patients leads to ICU-acquired weakness.
- ICU-acquired weakness increases healthcare costs by 30.5%.
- ICU-acquired weakness leads to more re-intubations, tracheostomies, and prolonged time on the ventilator.
- For sepsis patients, ICU-acquired weakness can increase time on the ventilator by 20 days.
These kinds of issues can have an extremely detrimental effect on patient outcomes, but they can also significantly increase the healthcare costs incurred by your ICU.
That being said, now that you know the consequences of failing to implement the ABCDEF Bundle, let’s review the financial benefits that these evidence-based practices can provide.
And if you’d like to learn more about the cost of not implementing these protocols, you should check out Episode 95 of my Walking Home From The ICU podcast.
What Are the Financial Benefits of the ABCDEF Bundle?
Once clinicians stop viewing the implementation of the ABCDEF Bundle as an unwanted expense and start seeing it as the investment it truly is, then more ICUs will begin to adopt these practices, and that’s a win-win-win for patients, staff, and hospital systems.
So, with that in mind, let’s take a look at how these evidence-based practices, such as early mobility and avoiding sedation, can boost your hospital’s bottom line, while also offering better care and outcomes for your patients.
Avoiding sedation has been proven to:
- Prevent/minimize delirium
- Decrease time on the ventilator
- Reduce the length of ICU and hospital stays
Early mobility has been proven to:
- Prevent/treat ICU-acquired weakness and diaphragm dysfunction
- Minimize time on the ventilator
- Reduce the length of ICU and hospital stays
- Increase the number of patients discharged home
- Decrease hospital-acquired infections by 60% with a 300% increase in mobility
- Decrease ventilator-associated pneumonia by 40% for each day mobility level is increased
Investing in adequate staffing has also been proven to directly decrease healthcare costs. A study from Brazil found it was cheaper to have physiotherapists in the ICU 24 hours a day rather than 12 hours a day.
In another study, an ICU increased its physical and occupational therapy staffing from two therapists to four, which increased the dose of early mobility provided to patients and decreased ICU length of stay by 3.6 days.
In addition, minimizing sedation alone has been proven to reduce healthcare costs. A study found that the PAD initiative in one hospital led to a 46% decrease in sedation and analgesia use. This resulted in saving $183,216 in drug costs and $1.2 million in savings for direct hospital costs.
The ABCDEF Bundle has also been shown to:
- Decrease healthcare costs by up to 30%
- Decrease ICU readmissions by 46%
- Reduce the incidence of delirium by 50%
- Increase patients’ chances of being discharged home by 36%
These incredible benefits were found, on average, even with low levels of compliance. It’s also been discovered that outcomes are dose-dependent, which means that the more teams adhere to an Awake and Walking ICU approach, the better outcomes will be.
A study from Johns Hopkins that evaluated the potential cost savings of implementing the practices found in the ABCDEF Bundle found that an investment of the 2023 equivalent of $114,455.85 resulted in net savings of $4,916,213.94.
In addition, a study from the Journal of Trauma Nursing found that in one ICU, the implementation of an early mobility program resulted in more than $8,000 in cost savings per patient.
As you can see, investing in these practices can have a major impact on a hospital’s bottom line, and many of these benefits can be achieved, even with low levels of compliance. However, the better the compliance, the better the outcomes, and chances are, greater compliance will result in even greater cost savings.
Unfortunately, the failure to support ICU teams with adequate staffing, education, and training is leading to a severe financial crisis within our hospitals and healthcare systems.
All things considered, now is the time for hospital systems to recognize the financial benefits of the ABCDEF Bundle. We must stop viewing its implementation as an “extra expense” and realize that it’s actually an investment in the health of patients, the well-being of clinicians, and the financial stability of the healthcare system.
Do you want to implement the ABCDEF Bundle in your ICU? We can guide you through the entire transformation, and we look forward to discussing your team’s needs. Please contact us here.




