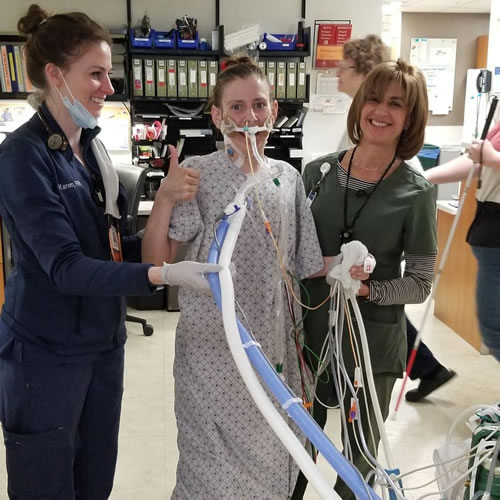History of the Awake and Walking ICU
The 1990s was an era of evolution in ICU critical care medicine. The ability to care for sicker patients with severe conditions such as acute respiratory distress syndrome (ARDS) was a new development. Patients were kept alive successfully on ventilators for longer periods of time and new treatments were being attempted.
As ARDS became a focus of new research, continuous sedation and paralytics entered the ICU. It seems managing the ventilator and caring for patients who were deeply sedated and paralyzed was just easier for the staff. It was also assumed that patients were as comfortable as they looked. In those early phases of ICU critical care research, little was known about the patient perspective and repercussions of prolonged deep sedation and immobility.
Polly Bailey was a nurse in a shock trauma ICU in Utah during the 1990s. Automatic deep sedation and paralytics for patients on ventilators were normal to her. These practices remained unquestioned until she started visiting a patient after she was discharged from the ICU. The patient, Joy, was a young mother in her 30s who had survived ARDS after weeks of deep sedation and paralytics. Polly was shocked to watch Joy spend a year being unable to walk up her stairs. She watched Joy’s husband help her with her bedpan and was shaken by her reports of cognitive disability and deep psychological trauma from her experiences under sedation.
At this point, Polly started to sincerely question if the price of saving these patients’ lives was worth it, given the lives they were forced to live after leaving the ICU. As a result, she was inspired to ask, “Do we have to cause patients to have muscular atrophy while on the ventilator? If patients aren’t sleeping under sedation, and they’re traumatized by sedation, what if we didn’t sedate them? What if we kept patients awake and moving while they’re on mechanical ventilation?”
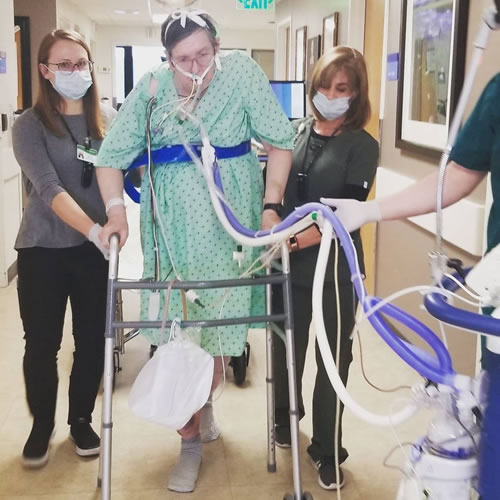
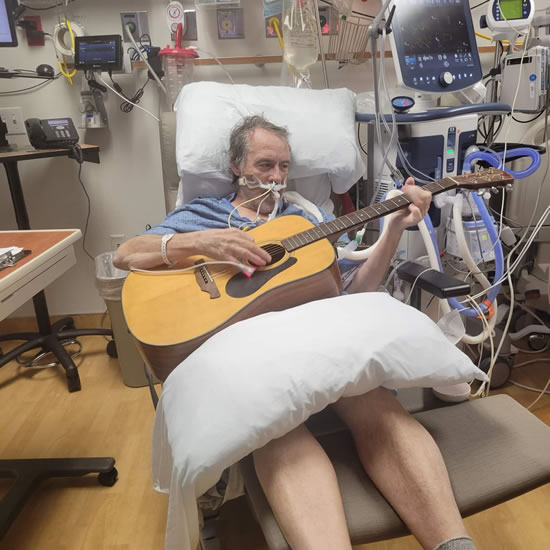
After having this realization, Polly presented her concerns and ideas to the medical director of her ICU, Dr. Terry Clemmer. Dr. Clemmer found validity in her concerns but was doubtful of her idea to avoid sedation and allow for early mobility in the ICU during mechanical ventilation. Still, Dr. Clemmer said, “I trusted her instincts. I knew Polly was a good nurse and trusted her to keep patients safe.”
As Polly started discontinuing sedation and mobilizing her intubated patients, they saw a significant difference in those patients’ outcomes. Without research to guide them, Polly was forging untrodden paths, yet the benefit of her approach was quickly clear. They found patients were able to get off the ventilator sooner and were able to be more functional during and after the ICU. However, despite the undeniable benefits of this approach, combating years of culture and misinformation among ICU clinicians was difficult. Change was slow in the shock trauma ICU.
Then, when a new respiratory ICU was started, Polly was given the opportunity to establish her approach as the standard practice. They recruited nursing home nurses without ICU experience or an inclination for deep sedation to train in their new ICU, and the new team learned the “Bailey Method,” which is the practice of allowing patients to wake up after intubation and promptly mobilize with the ventilator.
Surprisingly enough, many nurses who had fears and inhibitions about these changes (Episode 40) have since become her greatest allies and strongest forces for change. For example, Louise Bezdjian (Episodes 26 and 58) was a nurse with Polly in the shock trauma ICU. She hesitated to adopt her methods, but once she witnessed the prevention of patient suffering and harm, she was a devoted convert.
Polly and Louise have dedicated the past 30 years of their careers as nurse practitioners to the mastery of the “Bailey Method” in their medical-surgical ICU. In 2007, they published the first study demonstrating the safety and feasibility of ambulating patients with acute respiratory failure on mechanical ventilation. They have been the champions and guardians of this process of care throughout decades of changes.
This Awake and Walking ICU in Salt Lake City, Utah, has continued the practice of allowing nearly all patients to wake up after intubation and walk soon after. This standardization of care has persisted even during the trying COVID era, as they have maintained an Awake and Walking COVID ICU. (Episodes 44, 45, 86, 93) Their example demonstrates the power of unit culture and an interdisciplinary team approach, and their journey proves that changing perspectives, beliefs, and long-held traditions in medicine requires heart, hard work, and perseverance.
The dedication Polly and Louise have shown for preventing nosocomial harm through humane care has resulted in the saving and preservation of innumerable lives throughout their careers. Through their experiences, they have proven that the standardization of the “Bailey Method” is feasible for any team that desires to practice evidence-based medicine and humanize their ICU.
Today, there are many ICUs around the world that have standardized the “Bailey Method” and are working towards becoming Awake and Walking ICUs. ICU clinicians of all disciplines (Episodes 53, 59, 70, and 79) are daring to stand for best practices and leading their teams through the process of mastering the ABCDEF Bundle.
If you’re ready to lead your team into the future of ICU critical care medicine and want support from Awake and Walking ICU experts, we are here to help. Schedule a consultation today.