
Mastering the ABCDEF Bundle Is an Investment, Not an Expense

Learn about The Financial Benefits of the ABCDEF Bundle today!
This eye-opening presentation explains how creating an Awake and Walking ICU can provide significant cost savings.

Get instant access to our webinar on The Financial Benefits of the ABCDEF Bundle.
By clicking the above button, you agree to this site’s Privacy Policy. Your information is always kept safe and secure. You will also receive our monthly newsletter.
Do you want to create an Awake and Walking ICU, but you’re afraid it’ll be too expensive?
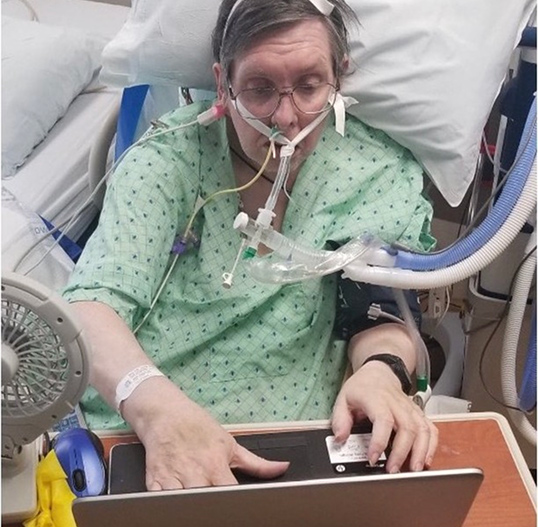
The evidence-based practices found in the ABCDEF Bundle can provide significant financial returns, and have been shown to:
- Prevent/minimize delirium
- Prevent falls in the ICU
- Decrease time on the ventilator
- Decrease ICU readmissions by 46%
- Reduce the incidence of delirium by 50%
- Reduce the length of ICU and hospital stays
- Decrease hospital-acquired infections by 60%
- Increase patients’ chances of being discharged home by 36%
Discover What Studies Have Revealed
- The ABCDEF Bundle has been shown to decrease health care costs by up to 30%.
- A PAD initiative in one hospital led to a 46% decrease in sedation and analgesia use, resulting in savings of $183,216 in drug costs and $1.2 million in savings for direct hospital costs.
- An estimate of the potential cost savings of implementing the practices found in the ABCDEF Bundle found that an investment of the 2023 equivalent of $114,455.85 would result in net savings of $4,916,213.94.
- In a trauma ICU, the implementation of an early mobility program resulted in more than $8,000 in cost savings per patient.
- Each unit increase in out of bed mobility in a medical ICU decreased time on the ventilator by 22% and time in the ICU by 5-11%.
- In a CVICU, an increase in physical and occupational staffing from 2 to 4 clinicians resulted in a 3.6 day decrease in ICU length of stay.
Can Your ICU Afford Not to Master the ABCDEF Bundle?
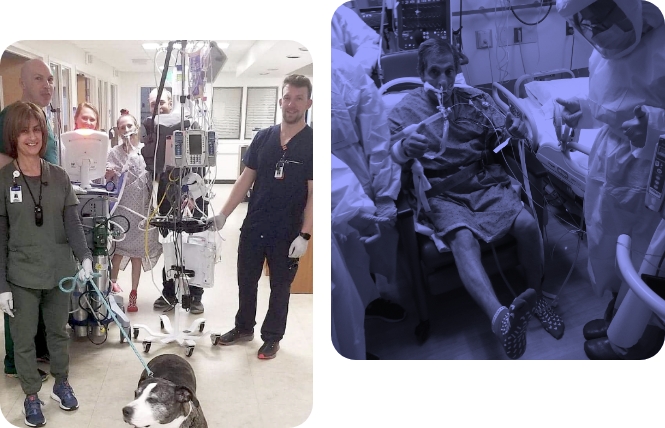
Failing to master the ABCDEF Bundle can significantly increase health care costs in many ways, including:
- Increased delirium
- Increased injuries to staff
- More time on the ventilator
- Increased workload for staff
- More hospital-acquired pressure injuries and falls
- Heavier psychological burden on staff, leading to burnout
- Discharges to care facilities for weeks or months of rehabilitation
- More hospital-acquired infections, such as hospital and ventilator-associated pneumonia, central line-associated bloodstream infections, and catheter-associated urinary tract infections

Who Is Kali Dayton?
Kali Dayton, DNP, AGACNP, is a critical care nurse practitioner, host of the Walking Home From The ICU and Walking You Through The ICU podcasts, and critical care outcomes consultant. She is dedicated to creating Awake and Walking ICUs by ensuring ICU sedation and mobility practices are aligned with current research. She works with ICU teams internationally to transform patient outcomes through early mobility and management of delirium in the ICU.
